Prevent
Whether mental illness or substance use disorders develop depends on a variety of social, biological, and neurological factors. However, since many of those factors are malleable, they can be targeted for prevention and health promotion efforts. Additionally, the Affordable Care Act included prevention as one of the 10 essential health benefits that must be covered by health plans, giving us the opportunity to engage the private sector to invest in behavioral health prevention and early intervention.
A range of prevention strategies could be implemented statewide in California, with diverse financial support that is broader than the current county behavioral health programs. After all, the savings generated by prevention investments can be enjoyed in both the private and public sectors. By providing public education about behavioral health and addressing key protective and risk factors in every community of the state, California can save lives, reduce suffering, and see a substantial return on its investment. According to 2018 state report on California’s use of federal SABG funding, evidence-based prevention strategies have returns on investment of up to 18:1, meaning for every $1 invested in prevention, $18 are saved due to reduced medical costs, increased productivity in work and school, reduced crime, and generally better quality of life.[i]
EDUCATE TO BUILD AWARENESS
Educating the public about the early signs of mental health and substance use disorder conditions and how to seek help is an effective public health approach to behavioral health prevention and promotion. Helping individuals learn about the early signs of behavioral health problems, the benefit of receiving treatment, and how to get treatment can help California shorten the time between the first sign of a problem and accessing help. Learning about behavioral health conditions and how common they are can also help reduce stigma and discrimination. However, providing information is not effective as a singular tactic and should be accompanied by additional prevention strategies, such as mentoring and skill building, to reduce risk and foster protective factors discussed next in this document.
Public education about behavioral health can be provided by a variety of entities, including schools, primary care providers, and providers in systems serving vulnerable individuals (e.g., child welfare, probation). Media campaigns that reach millions of people and can change attitudes and behavior are effective when thoughtfully designed and delivered. For instance, a RAND Corporation evaluation of county-funded mental health prevention campaigns in California demonstrated the potential we have to change actions and beliefs in our state.[ii] Participants in educational training programs conducted by the National Alliance on Mental Illness reported immediate improvements in knowledge about mental health and attitudes toward people with mental health challenges, including greater willingness to socialize with, live next door to, and work closely with individuals with mental illness. Distressed individuals who were exposed to their “Each Mind Matters” campaign were more likely to seek treatment. The counties’ “Know the Signs” campaign reached over half of all adults in California and raised their confidence in intervening with people at risk of suicide.
RAND evaluators suggested that California’s progress toward broader goals — including reducing suicide, improving early receipt of needed services, reducing discrimination, and avoiding some of the negative social and economic consequences associated with mental illness — will require a long-term commitment to a coordinated prevention and early intervention strategy that is continuously informed by population needs, evidence regarding promising and best practices, and indicators of program performance and quality.
In the case of substance use disorder prevention strategies using educational methods, the National Institute on Drug Abuse recommends that prevention programs for elementary school children target improving academic and social-emotional learning to address risk factors for drug abuse, such as early aggression, academic failure, and school dropout.[iii] For middle or junior high and high school students, prevention programs should increase academic and social competence. Prevention education can include resisting pressure to use drugs, looking at the intent behind advertising about drugs and alcohol, or developing other skills used in making healthy choices.
SUPPORT PROTECTIVE FACTORS & REDUCE RISK FACTORS
The evidence for prevention in behavioral health emphasizes how important it is to invest in reducing risk factors and boosting protective factors. According to the U.S. Office of Disease Prevention and Health Promotion:
“Health starts in our homes, schools, workplaces, neighborhoods, and communities. … Our health is also determined in part by access to social and economic opportunities; the resources and supports available in our homes, neighborhoods, and communities; the quality of our schooling; the safety of our workplaces; the cleanliness of our water, food, and air; and the nature of our social interactions and relationships. The conditions in which we live explain in part why some Americans are healthier than others and why Americans more generally are not as healthy as they could be.”[iv]
Research shows that the risk for mental health problems and substance abuse increases as the number of risk factors increases, and that protective factors may reduce the risk.[v] Risk factors make behavioral health problems more likely to occur, while protective factors reduce their likelihood. Evidence-based strategies to increase protective factors and reduce risk factors in behavioral health are numerous. Fortunately, national databases describe specific programs and service approaches that have been rigorously reviewed and found to be efficacious.[vi] Selecting which program or service approach to implement is based on collecting data to understand the needs of the target population and community priorities, and determining readiness and resources needed for organizations that will be involved to establish and sustain an organized prevention effort.
Based on research evidence, the tables below describe the youth risk and protective factors California should target to reduce the incidence of mental health problems and substance use disorders. They are organized by the domain in which they occur — the individual, family, and community levels.
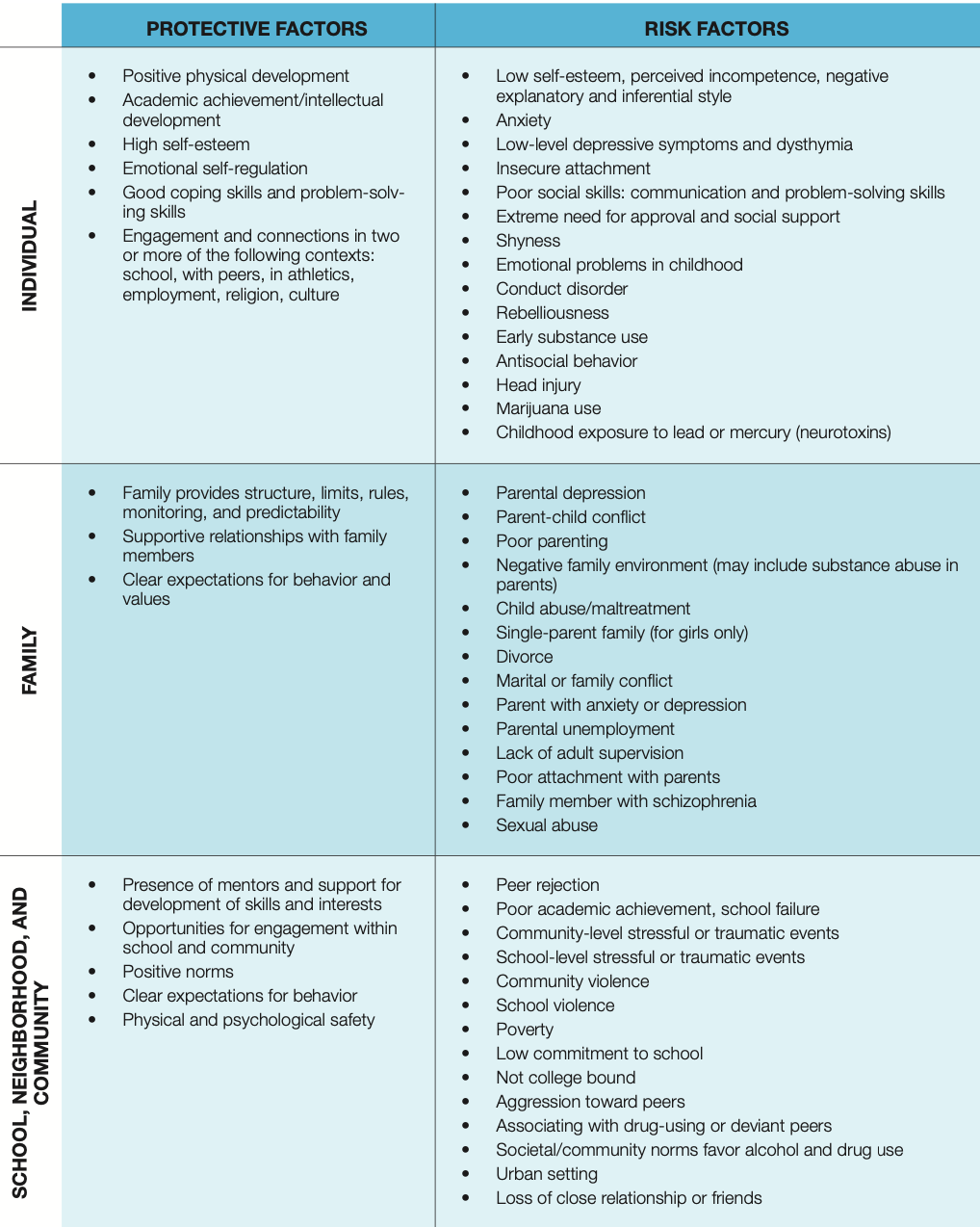
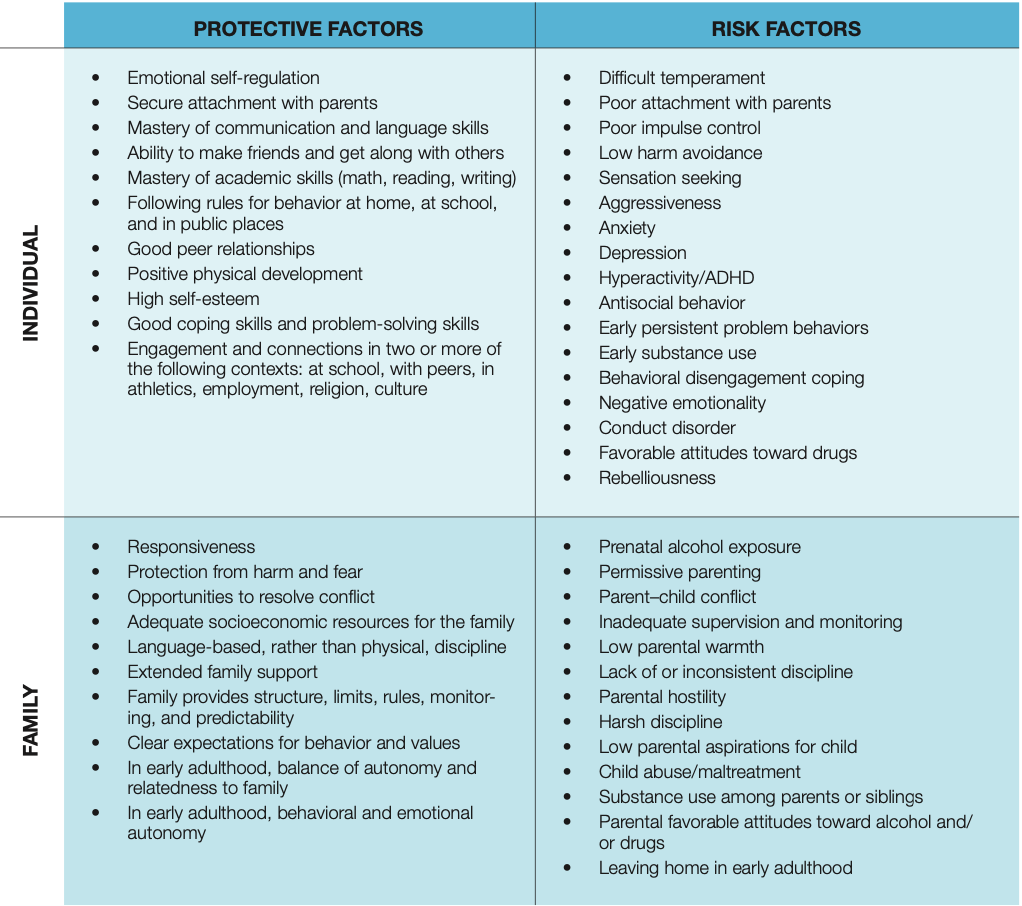
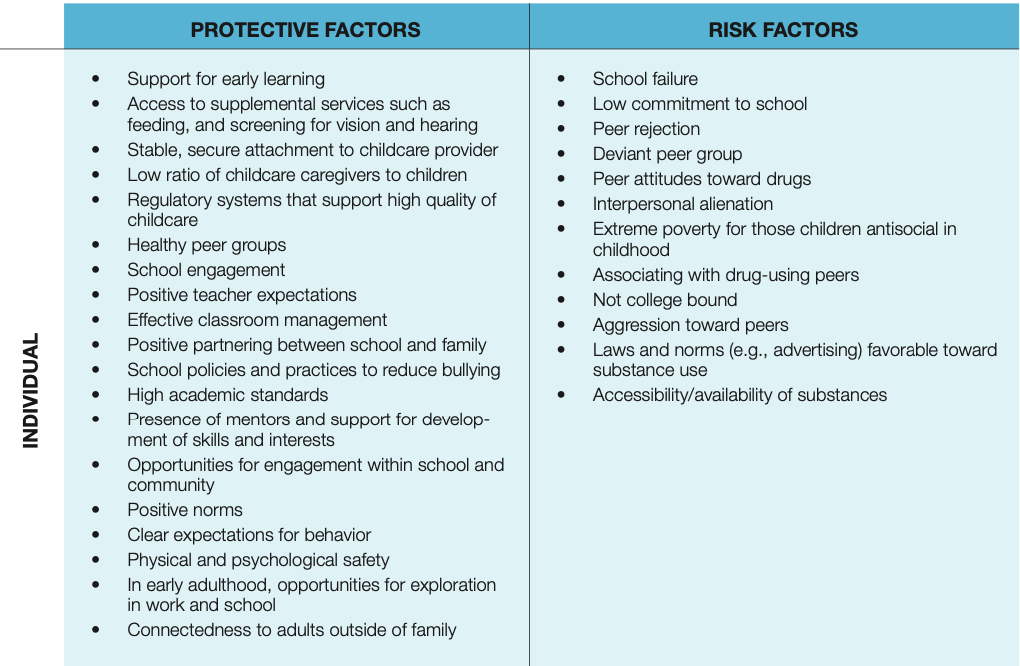
Citations:
[i] National Association of State Alcohol and Drug Abuse Directors, “Substance Abuse Prevention and Treatment (SAPT) Block Grant: Prevention Set-Aside Fact Sheet,” February 2019, https://nasadad.org/2019/02/sapt-block-grant-prevention-set-aside-fact-sheet/
[ii] RAND Corporation, “On the Road to Mental Health: Highlights from Evaluations of California’s Statewide Mental Health Prevention and Early Intervention Initiatives,” 2016, https://www.rand.org/pubs/research_briefs/RB9917.html
[iii] National Institute on Drug Abuse, “Lessons from Prevention Research,” 2014, https://www.drugabuse.gov/publications/drugfacts/les- sons-prevention-research
[iv] Healthy People 2020, “Social Determinant of Health,” Office of Disease Prevention and Health Promotion, 2019, https://www.healthy- people.gov/2020/topics-objectives/topic/social-determinants-of-health
[v] Youth.gov, “Risk and Protective Factors,” https://youth.gov/youth-topics/youth-mental-health/risk-and-protective-factors-youth, https:// youth.gov/youth-topics/risk-and-protective-factors
[vi] National Institute of Justice, Crime Solutions, https://crimesolutions.ojp.gov/; Youth.gov, Program Directory Search, https://youth.gov/ evidence-innovation/program-directory; SAMHSA, Evidence Based Practices Resource Center, https://www.samhsa.gov/ebp-resource-center


